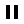Distal or subtotal pancreatectomy
When is surgery required?
Surgery is required to remove tumours, lumps or cysts in the pancreas that are cancerous, have a risk of becoming cancerous or those which are causing symptoms
What symptoms can be caused by tumours in the body or tail of the pancreas?
Tumours or cysts can compress or block the ducts of the pancreas, this may cause the area of the pancreas to die or atrophy (shrink). This can lead to enzyme deficiencises, which can lead to oily bowel motions or diabetes. These tumours can also cause pancreatitis, inflammation of the pancreas gland, which can result in pain and vomiting. If tumours become large they can press on advacent organs or blood vessels, such as the stomach or veins from the bowel or spleen.
What tests will need to be performed prior to surgery?
Most people will have a specialised pancreas CT scan of the abdomen. An MRI scan maybe required to look at the pancreas ducts and any cysts. If cancer is suspected then a biopsy or PET scan may be performed. Blood tests will be perfomed to check for diabetes and to assess fitness for surgery.
What type of anaesthetic is required for pancreatic surgery?
A full general anaesthetic will be required for pancreatic surgery. Sometimes an epidural or spinal anaesthetic is used to reduce the amount of painkillers required.
Will I need chemotherapy prior to surgery?
Neoadjuvant (pre-operative) chemotherapy is currently given for pancreatic cancer, when there is a risk that the tumour cannot be completely removed at surgery.
What does this distal pancreatectomy involve? Is it a Whipple procedure?
Operations on the body ot tail of the pancreas are called distal or subtotal pancreatectomy. These operations are different from a ‘whipple procedure’ which is performed for a tumour in the head of the pancreas.
Removal of the body and tail of the pancreas involves dividing the pancreas in the mid portion and removing the smaller triangular shaped portion of the pancreas. The artery and vein to the spleen are removed as they are very close to the pancreas and its lymph nodes. Because of this the spleen is also removed.
What is the function of the spleen?
The spleen filters the blood and provides an immune defense to some bacteria (bacteria with capsules)
Can I live normally without my spleen?
Yes, most people who have their spleen removed can live completely normally. Care has to be taken if you are having any minor surgical or dental procedures (extra antibiotics) and should you become unwell with fevers you will need to see your GP. People who have their spleen removed have regular vaccinations against the capsulated bacteria.
If part of my pancreas is removed will I be diabetic?
The risk of diabetes increases with the amount of pancreas removed. When the body and tail of the pancreas is removed, in people who do not have diabetes, the risk of diabetes is around 15%. Not all of these people will need insulin injections.
Can distal pancreatectomy or subtotal pancreatectomy be performed laparoscopically or robotically?
Yes, these operations can be performed with keyhole surgery unless there is a risk of tumour being left behind. Keyhole or minimally invasive surgery can be less painful and result in a quicker return to normal function. However, the aim of the surgery is always to completely remove a tumour and the associated lymph nodes. This should not be compromised by a minimally invasive operation.
What are the risks of surgery?
The general risks of any operation apply to distal or subtotal pancreatectomy. These include wound infection, chest infection, unexpected heart problems or stroke. The specific risks for this surgery include leakage from the pancreas, intra-abdominal collections, bleeding and pulmonary embolus .
A full explanation of this risks of surgery (personalised to your own condition and personal health) will be discussed with you prior to you giving consent to surgery.
How long will I need to be in hospital?
This will depend on your general health and fitness, as well as the extent of the tumour or cyst being removed. In general, if you have keyhole surgery you may be able to go home in 3-4 days. For conventional open surgery a 5-7 day stay can be expected. Should any complications of surgery occur the expected length of stay can be significantly increased.
How soon can I return to work?
It may take 4-6 weeks for you to feel well enough to return to work